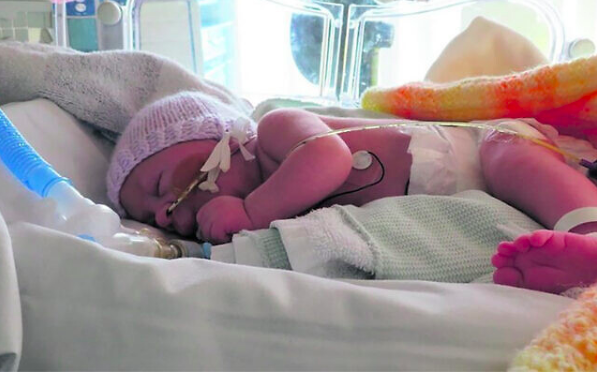
There’s something grimly familiar about the case of little Alta Fixsler, the brain-damaged toddler whose parents are contesting the decision of the Royal Manchester Children’s Hospital in England to withdraw her life-support treatment. She hasn’t eaten or spoken since she was born, tragically prematurely, a misfortune that left her with permanent brain damage. The hospital wishes to turn off her support but her parents want her to be transferred to a hospital in the United States — her father has an American passport — or to Israel — her parents are Israeli citizens, as is she — where the leading pediatric hospital has volunteered to take her.
The hospital trust has been supported by the courts where Mr Justice MacDonald was explicit that:
‘There is no requirement for the court to evaluate the reasonableness of the parents’ views before it embarks upon deciding what, objectively, is in the child’s best interests.’
The parents took the case to the European court, which refused to intervene. So now it’s down to the hospital to decide whether a brain-damaged little girl may go abroad to a hospital where she will at least have the chance of longer life, and certainly would die within her own community.
Israeli and US politicians have lobbied the hospital on the child’s behalf; the UK Foreign Office sniffily says that it will not entertain outside pressure on this matter. Fine; though I’d be a bit troubled myself about obliging the citizen of another country, even a child born here, to die on our terms. But how about simple humanitarianism?
We’ve been here before, that’s why it seems familiar: with Alfie Evans, the brain-damaged boy whose parents fought hard to give him a last chance of life by taking him to a hospital in Italy, the Bambino Gesu, which had offered to treat him. Their efforts were seen off by the courts on the basis. I wrote at the time about the hideous illogic of the argument; he couldn’t be transported to Italy because during the journey he would be ‘more vulnerable’, so he was forced to remain in Britain where the only option was for him to die.
We also, of course, had the case of Charlie Gard, a boy with a rare mitochondrial disorder whose parents wanted to give him the chance of an offbeat therapy available in New York; Great Ormond Street Hospital insisted that the boy’s condition was such that he should not travel; the upshot was that the courts agreed that he had to remain here to die.
Alta’s case is very similar, with the difference that Alta’s parents are Hasidic Jews and they argue that the courts are giving insufficient weight to their religious views that it is impermissible to end a life, unless the life involves great suffering, and to their rights as parents. In this case since the child cannot breathe unaided, she will die relatively quickly if the support is withdrawn.
Since the European Court of Human Rights refused to intervene, there are no further legal avenues the parents can explore. Her parents said: ‘We are heartbroken by this decision about our beautiful daughter, and we are exploring all available avenues to save her precious life.’
As with Alfie Evans, the chances of the little girl recovering are remote, but in a hospital in the US or Israel she may well live longer. Yet the courts are refusing to countenance the move. But there is no certainty whatever that she would feel any discomfort because she may not have the neurological capacity to feel pain.
What, in these circumstances, has the child to lose? She may live longer in Israel or the US; her parents want her to have whatever chance of life she can. Why should the British courts stop them? The medics here maintain she would undergo suffering if she travels, yet they provide insufficient proof — at least in the written judgment — that she would.
In this case, the pundits have not taken up arms against the parents and their supporters, whereas with Alfie Evans, some journalists had a particular animus against Alfie’s army because they seemed emotional and hostile to hospital staff. These people also appeared to especially dislike the Christian legal aid organization which supported the parents. Alta is Jewish and her parents have the support of Jewish hospitals and American and Israeli politicians; they are unlikely to be treated quite so contemptuously.
But I do question why religious views must come into the matter. Why is it not sufficient that a child’s parents wish her to have as much chance of life as possible, even if the chances of a cure are vanishingly small? Why must they be motivated by a specifically religious impulse? I happen to be strongly opposed to the withdrawal of feeding and hydration tubes from patients who rely on them for life, because I don’t think food and drink count as medical treatment (artificially maintained breathing is another question) but I don’t think of this as a religious, so much as a moral position which any unbeliever might share.
In this case the parents’ assertion of their right to prolong her life should not have had to include their religious beliefs. Religion (Christian Science excepted) doesn’t in these cases entail a peculiar position on medical ethics; just the normal impulse to do the best for a child. Making a case on the basis of the parents’ religion leaves at a disadvantage other parents arguing for their child without the benefit of religion. I’d say this case stands on the basis of natural justice.
In fact, I think Sajid Javid, the British health secretary, is quite amenable to these arguments. He will be sensitive to the fact that the child’s parents are Israeli citizens, even if she was born here; he will be aware of the fact that a global Jewish community supports the parents. But beyond that, he will recognize that Alta’s parents love her and have her best interests at heart. The medical experts in Israel are no less expert than those in Manchester; if they feel they can help her, it’s not for British pediatricians to insist she dies on their terms.
In all these cases — Alta, Alfie, Charlie — the hospital trusts are going beyond their remit and the judges beyond the terms of the Children Act 1989 under which they are obliged to act in the best interests of the child. If little Alta only has the option of dying sooner in Manchester rather than later in Israel or America, then it baffles me that a judge can consider that he is acting in her best interests to keep her here. If she is going to a reputable hospital — it is in fact outstanding — then let the child be taken abroad.
But perhaps, now that its authority has been upheld, Manchester University NHS Foundation Trust can afford to be magnanimous. They can, without loss of dignity, without seeming to capitulate to outside pressure, after consultation with their peers in Israel, let the child go. Medical and legal authoritarianism has its limits.
This article was originally published on The Spectator’s UK website.